Sarah
Doctors all said she would wake up wanting her breakfast the following morning, but I always had a feeling it wasn’t that straightforward.
My soon-to-be 8 year old daughter was very recently in hospital with ANEC (ANE?) after suffering from influenza A. She had seemingly usual virus symptoms and was ill off school with it on Monday 25th January 2016 but by late afternoon her temperature quickly spiked and she was yelling out to me that her legs were hurting and told me to take her to the hospital. I thought she was over-reacting (as she often does about things) but took her to the emergency GP surgery, instead. She became lethargic in the waiting room and vomited on the floor there. And couldn’t stay awake throughout the Dr’s examination. Her temp was over 41 deg C and I was told it’s a virus, to take her home and give paracetamol and ibuprofen and if no improvement in a couple of hours, to take her to the hospital.
After having the painkillers, she drifted off to sleep on the sofa and I waited for signs of improvement. Instead, she woke up confused and disorientated and hallucinating. Temperature still very high, I took her to our local hospital. She deteriorated quickly during the 4 hour wait to be seen by a Dr and it was only because she messed herself whilst waiting, but was too ill to even realize, that she was then seen. She drifted into unconsciousness almost the same time she was taken into a room for a Dr to examine her. Dr admitted her without delay because, besides everything else we had yet to have diagnosed, she was very dehydrated, with sunken eyes.
Doctors all said she would wake up wanting her breakfast, the following morning, but I always had a feeling it wasn’t that straightforward.
She was incontinent throughout the night, which began making Drs more concerned as to what might be wrong. She slept throughout, only to grizzle and moan, when they tried doing ob’s and wanted her to open her eyes to check her pupils. When they did manage to open her eyes the following day, to check, I noticed her left eye was turned totally inwards. I told the Drs and said that wasn’t normal; something was wrong. They said it might just be from where she’d slept so long as was tired. But I knew it wasn’t.
From the MRI they diagnosed encephalitis, she was transferred to a more specialized hospital Intensive Care Unit, where her condition was changed to acute necrotizing encephalopathy.
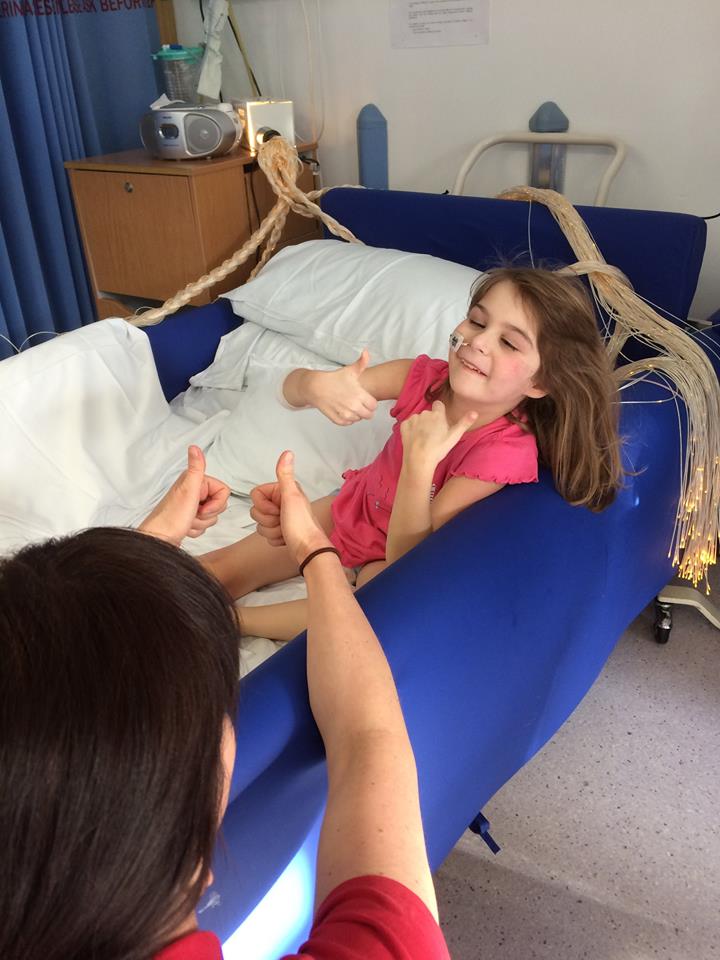
Her vitals were always ok…though they had her on a barrage of treatment. Antiviral’s, Tamiflu, steroid, antibiotics, clonidine and chloral and she had an immunoglobulin transfusion. When she did start to come round, she would thrash around in the bed so much, it made all of her skin very, very sore. They ordered in a special padded bed for her and a special circulating-air mattress, and even special silk sheets, to try to soothe her red and sometimes bleeding skin.
Initially, during the acute stage of the illness, the neurologist gave a 30% chance of survival and said the brain damage was such that, should she survive, the effects from it would be devastating. She later had a 2nd MRI, which showed improvement. I’m not sure how her brain lesions had improved, as I didn’t think brain cells could rejuvenate, unless it just rewired itself, but the signs were so much better than previous.
Sarah has since made remarkable recovery and was discharged home on 14th March, 6 weeks after hospital admittance. When she first came round from her illness, she didn’t seem to know who we were, but was then able to blink to reply to yes/no questions, or squeeze our hands for yes/no questions. Through hospital therapy, she learned to talk and eat and walk again.
She has some balance problems and fine motor skills problems, has been left with a deep, husky voice, swallowing issues, especially when drinking fluids, tremors and has a younger character than her peers. She has some behavioral problems going on, for examples, she can get very frustrated and very angry. Sleeping on her own as become a challenge, as she jolts awake when drifting off. She jumps and wakes herself up a lot, so I have to hold her down.
We are still in early days, I suppose, as far as complete recovery goes. This is all still so very new, very raw, and very upsetting and confusing as to how this happened. It still hasn’t quite sunk in, with me. She has tested negative for the mutated gene RANBP2, but genetics just contacted us and requested permission for further genetic testing to be carried out, so another long wait. I have no idea what they are looking for.
They can put man on the moon but they don’t know enough about ANEC (or ANE) and even the ‘treatment’ administered to my daughter was all just a guessing game, they said. I forget how many times I was told “We don’t know. It’s a case of wait and see”.
The hospital also told me it’s incredibly rare! Is it really? Or, is it just that it’s not recognized enough, due to lack of research and funding into that?
I keep crying for the daughter I’ve lost, as I don’t think she’ll ever be quite “my Sarah” ever again. However, I do thank God for her recovery, so far !!! She’s my little fighter and is my hero!
